Prescription Drugs
When lifestyle changes aren’t enough, the next step may be to take medicine. Your health care provider can tell you about special drugs for OAB.
There are several drug types that can relax the bladder muscle. These drugs, like anti-muscarinics and beta-3 agonists, can help stop your bladder from squeezing when it’s not full. Some are taken as pills, by mouth. Others are gels or a sticky transdermal patch to give you the drug through your skin.
Anti-muscarinics and betta-3 adrenoceptor agonists can relax the bladder muscle and increase the amount of urine your bladder can hold and empty. Combination drugs, like using both anti-muscarinics and - betta-3 adrenoceptor agonists together may help control OAB when one option alone isn’t working.
Your health care provider will want to know if the medicine works for you. They will check to see if you get relief or if the drug causes problems, known as side effects. Some people get dry mouth and dry eyes, constipation, or blurred vision. If one drug you try doesn't work, your health care provider may ask you to take different amounts, give you a different one to try, or have you try two types together. Lifestyle changes and medicine at the same time help many people.
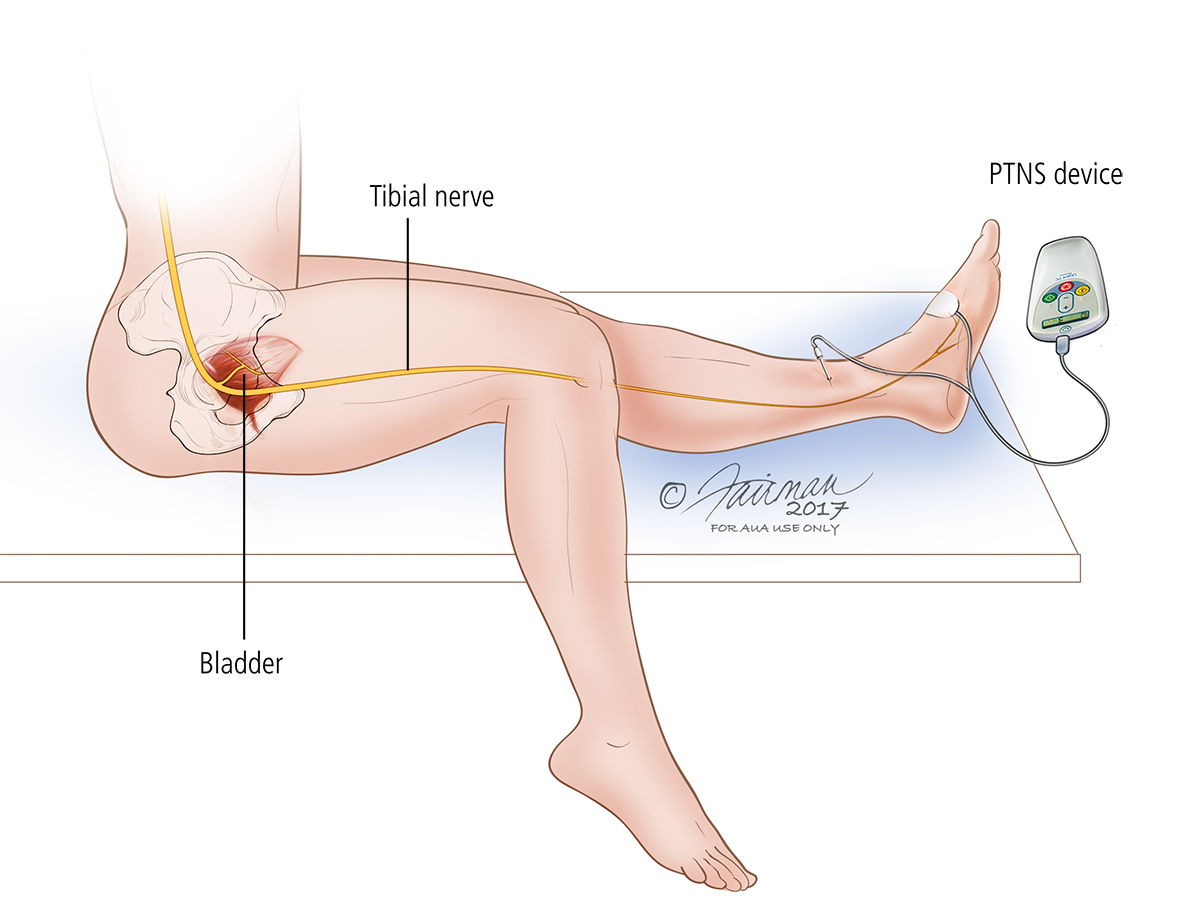
Bladder Botox Treatment
If lifestyle changes and medicine aren’t working, injections may be offered. A trained urologist for men and women, or a female pelvic medicine & reconstructive surgeon (FPMRS) can help with this. They may offer Bladder Botox Treatment.
Botox works for the bladder by relaxing the muscle of the bladder wall to reduce urinary urgency and urge incontinence. It can help the bladder muscles from squeezing too much. To put botulinum toxin into the bladder, your doctor will use a cystoscope passed into the bladder so the doctor can see inside the bladder. Then, the doctor will inject tiny amounts of botulinum toxin into the bladder muscle. This procedure is performed in the office with local anesthesia. The effects of Botox last up to six months. Repeat treatments will be necessary when OAB symptoms return.
Your health care provider will want to know if the botulinum toxin treatment works for you. They will check to see if you get relief, or if you aren’t holding in too much urine. If urine is not releasing well, you may need to use a catheter temporarily.



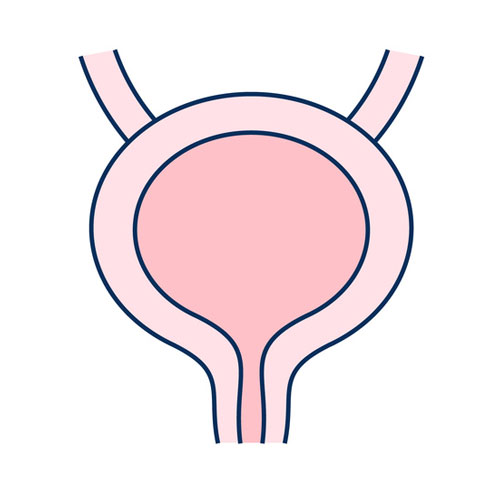 Normal Bladder
Normal Bladder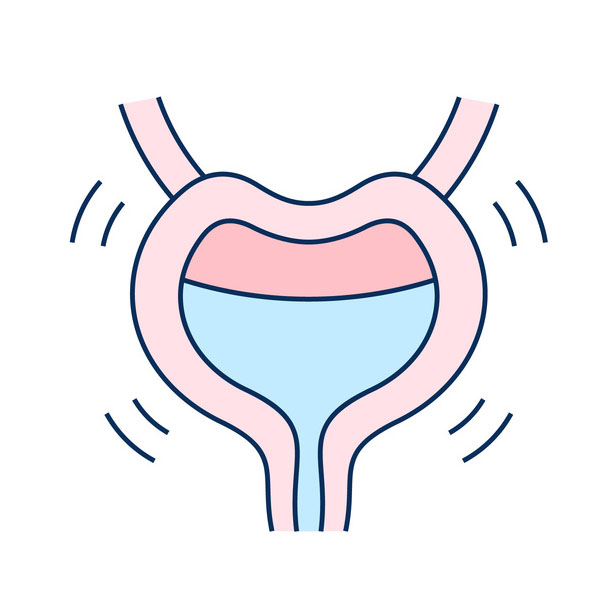 Overactive Bladder
Overactive Bladder